Many people drink alcohol and use drugs because they are depressed or become depressed as a result of prolonged substance abuse. Depression and addiction have a toxic, cyclical relationship that rips apart families, ruins careers and destroys lives. For many alcoholics and people with drug addictions, uncovering this link is key to making progress during rehab and maintaining sobriety following treatment.
Do you have problems with depression and addiction — Contact us right away at 772-774-3872.
The Prevalence of Co-Occurrence
We’ve all dealt with varying levels of depression throughout our lives. It can be difficult for a person to differentiate between the normal occurrence of depression and a depressive disorder. Due to this and several other factors, people struggling with depression don’t often seek any sort of treatment for their condition. As a result, many turn to alcohol or illicit drugs to try to feel better. This is a very common path toward substance abuse and addiction for millions of Americans and others around the world.[1],[2]
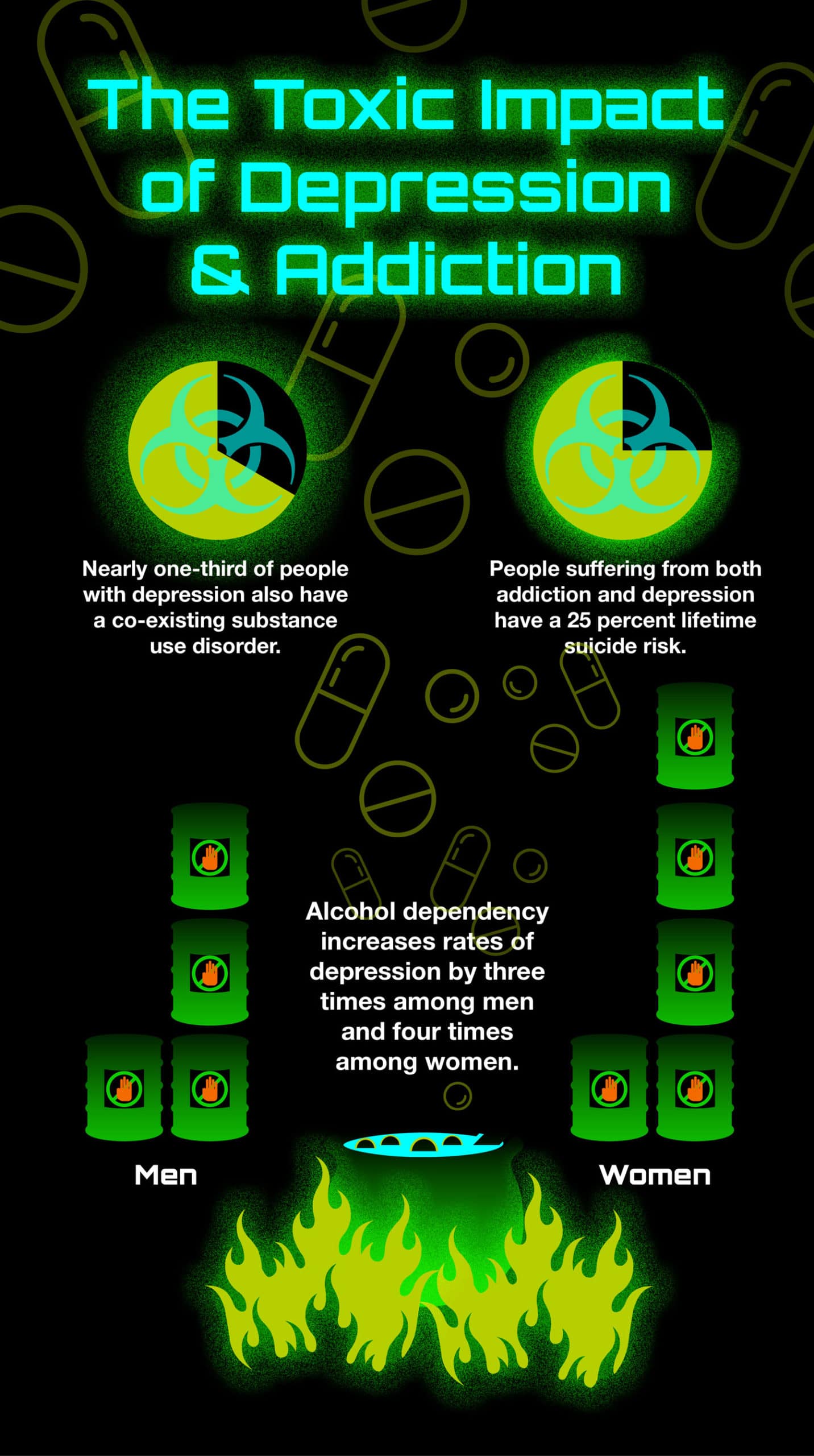
Though in many cases it is impossible to know which condition came first, women often develop depression first and while men more frequently struggle with addiction initially.[4] Overtime, the symptoms of both conditions collide, worsening both the depression and the addiction and creating a more difficult path for treatment.
Overlapping Risk Factors for Each Condition
It’s very common for addiction and mental illness to co-occur. According to the National Alliance on Mental Illness, approximately 50 percent of individuals with severe mental disorders also struggle with substance abuse. An estimated 37 percent of alcohol abusers and 53 percent of drug users have at least one mental illness.[5] Part of the reason that these conditions co-occur so frequently is because of the overlapping risk factors. The things that make a person more likely to abuse drugs or alcohol and develop an addiction are very similar to the characteristics that make a person more likely to struggle with a mental illness:[6],[7]
- Genetic Vulnerabilities: A person whose family has a history of addiction or mental illness is more susceptible to developing either condition
- Environmental Triggers: Stress, trauma and early exposure to drugs and/or alcohol are risk factors for both mental illness and substance use disorders
- Affects Similar Brain Regions: Mental illness and substance abuse impact some of the same areas of the brain, including the reward system and circuits linked to stress control and response
- Poverty: Multiple studies have linked low socioeconomic standing to both addiction and mental illness
The Compounding Problems of Depression and Addiction
By themselves, both depression and addiction present difficult challenges for individuals living with either condition. When they are combined, the cumulative effects of both conditions can be debilitating, life-altering and potentially fatal. For some, depression creates such an emotional low that the only way patients think they can feel better is through the use of mind-altering substances. While this may be effective in the short-term, it will be ineffective and lead to greater levels of depression in the long-run. A person who continually abuses drugs or alcohol to improve symptoms of depression weakens her ability to self-manage these symptoms and creates a dependency.

 It often begins innocently enough. A person is feeling down and figures a glass of wine will quickly make things better. That glass of wine turns into a bottle, then to two bottles, and so on. As this pattern continues, the individual will find that the only way that she can avoid feelings of depression is through use of drugs and/or alcohol. But the depression will inevitably return, likely packing a more powerful punch. Then more drugs or alcohol will be needed for temporary relief, and the cycle grows more and more dangerous with time.[8],[9]
It often begins innocently enough. A person is feeling down and figures a glass of wine will quickly make things better. That glass of wine turns into a bottle, then to two bottles, and so on. As this pattern continues, the individual will find that the only way that she can avoid feelings of depression is through use of drugs and/or alcohol. But the depression will inevitably return, likely packing a more powerful punch. Then more drugs or alcohol will be needed for temporary relief, and the cycle grows more and more dangerous with time.[8],[9]
In the end, you have a person who is struggling with depression and addiction without any idea how to overcome either condition. In many cases, this pattern continues until one or more negative life consequences forces change. It’s important for people to be aware of the signs of both conditions so that they can monitor themselves and those closest to them.
Incessant self-medication with drugs or alcohol interrupts the body’s natural production of dopamine, the neurotransmitter responsible for pleasure. Dopamine is released in high amounts when drugs or alcohol are introduced to the body, and repeated exposure may lead to the brain ceasing its natural production.
The Problem of Undiagnosed Depression
 Perhaps the most common reason why depression and addiction co-occur so often is because of how frequently depression goes undiagnosed and untreated. The fact is that the majority of people with depression or any other sort of mental illness do not seek or receive treatment.[10] In most cases, it’s because they believe it won’t be effective, they have limited access, they can’t afford it, they don’t feel they need help or they don’t want to deal with any negative stigma.[11]
Perhaps the most common reason why depression and addiction co-occur so often is because of how frequently depression goes undiagnosed and untreated. The fact is that the majority of people with depression or any other sort of mental illness do not seek or receive treatment.[10] In most cases, it’s because they believe it won’t be effective, they have limited access, they can’t afford it, they don’t feel they need help or they don’t want to deal with any negative stigma.[11]
Untreated depression leads to worsening symptoms of depression, suicidal thoughts and increases the risk of contracting other medical conditions. It can also lead to ruined relationships, problems at work or school and make it difficult to accomplish basic tasks in your life. This in turn can lead to even greater depression, to the point where some people may decide that they want to entirely drown out their feelings with drugs or alcohol.
Dual Diagnosis Treatment Challenges
One of the largest treatment obstacles facing individuals with dual diagnoses is lack of qualified professionals or sufficient facilities. Not all addiction rehab facilities are staffed with cross-trained addiction care professionals who can treat both addiction and mental illness. Though co-occurring disorders have existed for quite some time, they have only recently begun to be studied extensively over the past 30 years. Historically, there have been three different treatment strategies for dual diagnoses:
People with dual diagnoses frequently present more severe symptoms of both conditions than people with a single diagnosis. Additionally, treatment is less effective in dual diagnosis patients, and they are more likely to relapse following treatment.[12] Traditionally, the most common type of treatment for these patients was sequential. Many clinicians believed (and some still believe) that in order for one condition to improve, that the other had to be resolved. In many cases, the existence of one condition along with the other caused healthcare professionals and addiction treatment specialists to deem that a patient may not be a good candidate for treatment.
“Recent research has shown that the most effective way to treat dual diagnosis patients is with concurrent treatment.”
When a facility is staffed with healthcare professionals who can treat both conditions, it can minimize any potential conflicts between treatment strategies at one facility vs. another. This method is especially helpful in patients with persistent symptoms who require intensive or continuous care. Integrated care is more convenient for patients, reduces isolation by including them in the mainstream addiction population and likely costs less than having to be treated at multiple facilities.[13]
Specific Treatment Approaches
Several methods exist for treating depression and addiction. While research is still ongoing into which specific methods are most effective, current research has begun to paint the picture:[14],[15]
- Medication: There are several medications that have been determined to be effective in the treatment of opioid and alcohol addiction and for treating several mental illnesses. However, many of these medications have not been tested in dual diagnosis populations, so any potential dangers are unknown
- Cognitive Behavioral Therapy: This approach has proven to be effective in the treatment of both mental illness and addiction. It is a helpful tool because it begins the process of patients unlearning unhealthy preconceived notions about their conditions and learning new, healthy behaviors
- Therapeutic Communities: Community lodges, inpatient facilities and other types of therapeutic communities have become increasingly popular for the treatment of addiction and mental illness. These communities are helpful in the resocialization of patients to prepare them for sustained success in recovery
A Personalized Treatment Strategy is Essential

Whether a person is struggling with addiction, depression or a combination of the two, he or she will require a unique rehab strategy. There is no standardized level of addiction care or mental health treatment that is effective on all patients. Every person who enters treatment has differing levels of severity in his or her addiction and mental illness, in addition to having a unique family history and specific environmental triggers to overcome. A treatment strategy that accounts for all of these personal differences and others is critical to success.[16]
For some, cognitive behavioral therapy will prove extremely effective. Others may do better in group counseling or with activity-based therapies. Different approaches will have varying levels of success on patients based on their specific needs and challenges. Treatment should also account for the damage caused by substance abuse and mental illness. It may be necessary to help patients rebuild relationships with families, relearn life skills and improve physical fitness.
In addition, many dual diagnosis patients need to be educated about addiction and/or mental illness, how the conditions interact with one another and healthy ways to cope with inevitable mental distress. Aftercare services are also helpful in providing patients with a safety net and a system of accountability following treatment.
Behavioral Health Centers offers a comprehensive addiction treatment program that helps patients with dual diagnoses gain control over their conditions. We provide patients with a healing atmosphere, compassionate addiction therapists, knowledgeable medical staff and world-class mental health experts. Our top priority is to help our patients find their way to healthy, sober living. If you or a loved one is struggling with depression and addiction, please call us today at 772-774-3872.
[1] https://www.ncbi.nlm.nih.gov/pubmed/2232018 [2] https://www.ncbi.nlm.nih.gov/pubmed/9107147 [4] https://archives.drugabuse.gov/NIDA_Notes/NNVol12N4/Gender.html [5] https://www2.isu.edu/irh/projects/better_todays/B2T2VirtualPacket/MentalHealthMentalDisorders/NAMI%20-%20Dual%20Diagnosis.pdf [6] https://www.apa.org/about/gr/issues/substance-abuse/comorbid.pdf [7] https://www.apa.org/news/press/releases/2005/03/low-ses.aspx [8] https://www.everydayhealth.com/depression/symptoms.aspx [9] https://www.ncadd.org/about-addiction/signs-and-symptoms/signs-and-symptoms [10] https://www.scientificamerican.com/article/most-depressed-adults-in-the-u-s-remain-untreated/ [11] https://www.ncbi.nlm.nih.gov/pubmed/22854096 [12] https://www.drugabuse.gov/publications/research-reports/comorbidity-addiction-other-mental-illnesses/how-should-comorbid-conditions-be-treated [13] https://pubs.niaaa.nih.gov/publications/ahrw20-2/076-080.pdf [14] https://www.drugabuse.gov/publications/research-reports/comorbidity-addiction-other-mental-illnesses/how-should-comorbid-conditions-be-treated [15] https://www.drugabuse.gov/publications/research-reports/therapeutic-communities/what-are-therapeutic-communities [16] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4654192/








